For decades, fertility has largely been framed as a women’s health issue. But science tells a very different story. Male factors contribute to nearly 50% of fertility challenges, either alone or combined with female factors.
If conception is taking longer than expected, evaluating both partners early can save time, emotional stress, and unnecessary treatments. Supporting male fertility is not just helpful, it is essential.

Why Male Fertility Is Declining
Over the last 40–50 years, global sperm counts have declined significantly. While research is ongoing, several consistent contributors are emerging.
Environmental Toxins
Exposure to endocrine-disrupting chemicals can negatively impact sperm production and hormone signaling. These include:
- Plastics (BPA, phthalates)
- Pesticides and herbicides
- Heavy metals
- Air pollution
These compounds can disrupt testosterone production and increase oxidative stress in the testes.
Lifestyle and Metabolic Health
Modern lifestyle patterns strongly influence sperm quality:
- Poor sleep quality
- Processed food diets
- Insulin resistance and metabolic syndrome
- Excess alcohol use
- Smoking and vaping
Sperm production is highly energy-dependent, meaning mitochondrial health and metabolic health directly influence sperm quality.
Chronic Stress
Stress increases cortisol, which can suppress testosterone production and impair sperm formation. Chronic sympathetic nervous system activation also increases inflammation and oxidative damage.
Heat Exposure
Sperm production requires temperatures slightly below core body temperature. Regular exposure to heat can reduce sperm count and motility.
Common sources include:
- Hot tubs and saunas (frequent use)
- Heated car seats
- Laptops on the lap
- Tight underwear

What Men Should Get Tested
A comprehensive male fertility evaluation should go beyond a basic semen analysis when possible.
1. Semen Analysis (Foundation Test)
Evaluates:
- Sperm count
- Motility (movement)
- Morphology (shape)
- Volume
If abnormal, repeat testing is usually recommended because sperm production cycles every ~70–74 days.
2. Hormone Testing
Helpful markers include:
- Total and free testosterone
- LH and FSH
- Estradiol
- SHBG
- Prolactin
These help determine if fertility challenges are testicular, hormonal, or systemic.
3. Advanced or Functional Considerations
Depending on history and presentation:
- Sperm DNA fragmentation
- Oxidative stress markers
- Metabolic markers (insulin, glucose)
- Thyroid screening (if symptomatic)
- Nutrient status (vitamin D, zinc, selenium)
Evidence-Based Ways to Improve Male Fertility
1. Optimize Nutrition
Key nutrients for sperm health include:
- Zinc
- Selenium
- Omega-3 fatty acids
- CoQ10
- Folate
- Vitamin D
- Antioxidants (vitamin C, E, glutathione support)
A whole-food, anti-inflammatory diet supports hormone production and reduces oxidative damage to sperm DNA.
2. Improve Sleep
Testosterone is largely produced during sleep. Men consistently sleeping less than 6–7 hours often have lower testosterone and poorer sperm parameters.
3. Support Metabolic Health
Maintaining healthy insulin levels and body composition improves hormone balance and sperm production.
4. Reduce Toxin Load
Practical steps:
- Switch to glass or stainless steel food storage
- Filter drinking water
- Choose cleaner personal care products
- Reduce pesticide exposure when possible
- Avoid smoking tobacco and/or marijuana
5. Manage Stress
Stress reduction is not optional in fertility care. Helpful tools include:
- Exercise
- Breathwork
- Meditation
- Nervous system regulation practices
6. Avoid Excess Heat Exposure
Simple changes can help:
- Avoid frequent hot tub use
- Limit laptop use directly on lap
- Choose breathable underwear
Take breaks from prolonged sitting
Fertility Is Not Just a Female Issue
This is one of the most important mindset shifts in modern fertility care. When both partners are supported, outcomes often improve faster and more sustainably.
Men often want to help but don’t always know what to do or where to start. That’s where targeted, actionable guidance becomes powerful.
A New Tool for Male Fertility Support: Juno
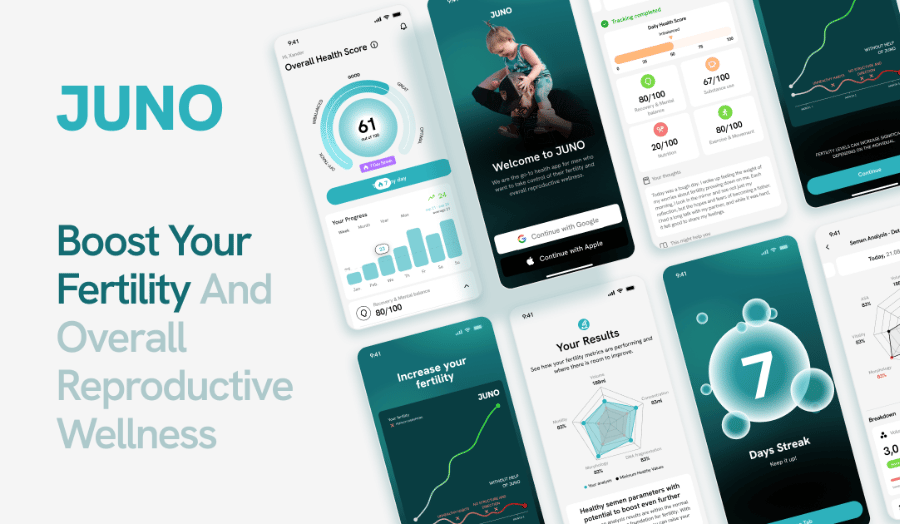
Fertility success is built on daily habits — Whole food nutrition, proper supplementation, stress management, sleep, non-toxic living, and movement all directly impact sperm quality.
Juno is designed specifically to help men take action on the factors that influence sperm health most.
Juno is the #1 app to improve sperm health and increase your chances of conceiving within 30 days. It helps men take action on evidence-based lifestyle changes, including sleep, nutrition, physical activity, stress, heat exposure, and other daily factors that contribute to sperm quality. Designed with urologists and grounded in the latest research in reproductive health, Juno turns daily habits into faster progress toward conception.
Try for free or use DRKELA10 for 10% off Juno Premium.
Final Thoughts
Fertility is a shared journey. When male fertility is evaluated and supported early, couples often:
- Reach answers faster
- Improve treatment outcomes
- Reduce emotional and financial strain
Supporting sperm health is not just about conception; it is also linked to long-term male health, hormone balance, and metabolic wellness.
The more we normalize male fertility care, the more complete and effective fertility treatment becomes.
Written by:

Dr. Kela Smith, PhD, DNM
Fertility and Hormone Expert
The Hormone Puzzle Society™
www.hormonepuzzlesociety.com
This blog/post is sponsored by Juno, a brand I genuinely recommend to my patients and use personally and have since they were founded.
These statements have not been evaluated by the Food and Drug Administration. This product is not intended to diagnose, treat, cure, or prevent any disease.
To learn more about my services or to book a telehealth appointment visit www.hormonepuzzlesociety.com.
Salas-Huetos A, et al. (2019). Adherence to the Mediterranean diet is positively associated with sperm motility and concentration. Human Reproduction.
Agarwal A, et al. (2014). Role of oxidative stress in male infertility. Reproductive Biology and Endocrinology.
Vaamonde D, et al. (2012). Physically active men show better semen parameters and hormone profiles than sedentary men. European Journal of Applied Physiology.
Janevic T, et al. (2014). Relationship between life stress and semen quality. Fertility and Sterility.
Jurewicz J, Hanke W. (2011). Exposure to environmental pollutants and semen quality. International Journal of Occupational Medicine and Environmental Health.

