Written by Guest Blogger: Jessica Manns, an embryologist and the creator of Explaining IVF.
In vitro fertilization (IVF) refers to the process of retrieving eggs from a woman’s ovaries, fertilizing them in a laboratory, and ultimately transferring any resulting embryo(s) to a woman’s uterus. Each step of the IVF process plays an important role in the overall success of the cycle. A successful IVF cycle results in a healthy live birth. In this guide, we will discuss how an embryo’s rate of development and grade, or morphology,
are recorded and how these factors can affect an embryo’s chance of success.
Once embryos are fertilized in the IVF lab, they are given a few days to develop inside a culture medium in an incubator. During this time, an embryo should develop from one cell (a fertilized egg) to over one hundred cells. Embryo development occurs through a process known as mitosis, or cell division.
Not all embryos develop at the same pace, and each has a unique physical appearance. Embryologists can estimate an embryo’s chance of success based on how quickly it develops and its morphology. Of course, these are only two factors to consider when calculating an embryo’s chance of success. For example, an embryo’s appearance does not guarantee that its cells contain the right amount of DNA. Further, embryo grading is subjective, which means that it can vary from person to person.

Embryo Development
Though some IVF labs may follow a different timeline, embryos should generally follow a basic developmental timeline similar to what is outlined in the table below. Keep in mind that some clinics do not culture embryos to day 7.
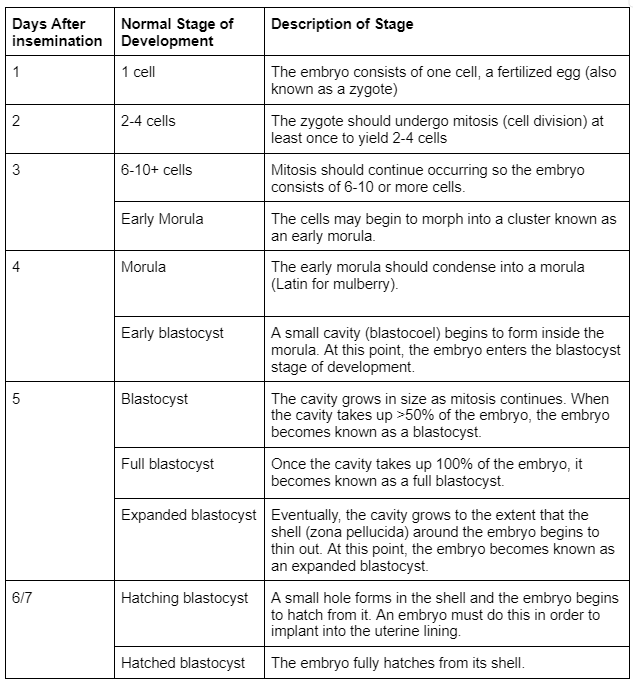
Embryos that are delayed in development do tend to yield lower overall success rates, though they do have the potential to result in healthy live births. For example, embryos that develop to the expanded blastocyst stage on day 5 yield higher success rates than embryos that do not develop to this stage until days 6 or 7.
An embryo’s appearance can be recorded at any stage of development. However, most clinics do not grade embryos until 3, 5, 6, and/or 7 (if your clinic cultures to day 7) days after insemination.
Day 3 Grading
Some clinics do not observe or grade embryos on day 3. If they do, day 3 embryo grading is usually based on three criteria (this can also vary between clinics):
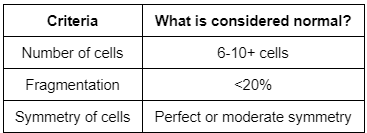
Not surprisingly, a large study found that day 3 embryos yield the highest success rates when they consist of 8 cells, 0% fragmentation, and perfectly symmetrical cells. At best, the transfer of a single day 3 embryo has roughly a 25-30% chance of resulting in a live birth.
Blastocyst Grading
Embryo grading becomes very different once an embryo reaches the blastocyst stage of development. At this point, an embryo is typically graded based on three criteria:
- Stage of development. Most clinics use a numbering (Gardner scale) or lettering system to record an embryo’s stage of development (see table below).
- Appearance of its inner cell mass (ICM). This small cluster of cells ultimately develop into the baby. Most clinics grade ICMs on an A, B, C (sometimes D) scale, with A being the highest grade. An ICM with an A grade is compact and circular, while an ICM with a C (or D) grade is often not compact or is absent.
- Appearance of its trophectoderm (TE). The TE cells line the shell of the embryo and ultimately develop into the placenta. Like ICMs, TEs are often graded on an A, B, C (sometimes D) scale, with A being the best. A TE with an A grade consists of many uniform cells with no gaps, while a TE with a C (or D) grade consists of few to no cells with many gaps.
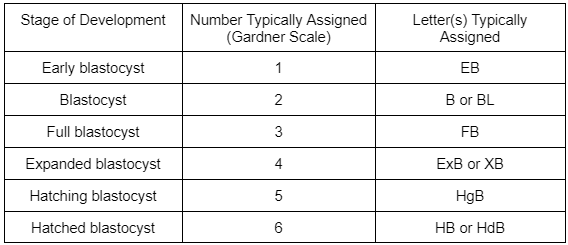
For example, an expanded blastocyst that has a perfect looking ICM and fair looking TE would be graded as a 4AB. A hatched blastocyst with a poor looking ICM and fair looking TE would be graded as a 6CB.
The higher an embryo’s quality, the higher its chance of resulting in a healthy live birth. For example, embryos with an A grade ICM and/or TE have a ~50% chance of resulting in a live birth, while embryos with a C grade ICM and/or TE have a 25% chance of resulting in a live birth.
Final Thoughts
An embryo’s rate of development and morphology are two factors that contribute to its overall success rate. However, there are other factors that must be considered when calculating an embryo’s chance of success, as well. Also keep in mind that embryo grading is subjective and may vary from person to person. For these reasons, I recommend not overthinking an embryo’s chance of success based solely on its rate of development and grade, though these factors can help determine the best embryo for transfer if preimplantation genetic testing is not performed.
Guest Blogger,
Jessica Manns

Jessica is an embryologist and the creator of Explaining IVF. She created Explaining IVF to help people undergoing IVF understand their procedures and other important information. As a growing field, IVF and infertility have become complex topics that aren’t always easy to understand. She likes to break everything down to make it more understandable to people so they can make informed decisions about their treatment. She lives in Pittsburgh, PA and enjoys traveling and spending time with her friends and family.
P.S. Catch Jessica’s interview in this week’s episode of The Hormone P.U.Z.Z.L.E Podcast – Understanding IVF. You can also find the episode on this podcast page as well as Spotify, and Stitcher. Don’t forget to subscribe, follow, and write us a review on Apple Podcast (if you LOVE it).

